By Rob Geyer, Chief Executive Officer of Reta Trust
 May 2018 – The top stories in American healthcare continue to focus on our ever-increasing healthcare costs—costs that are nearly double those of other high-income countries while outcomes fall short on many population health measures[1]. And with no end to this upward spiral in sight, employers are grappling with how to continue providing their employees with high quality, affordable healthcare without breaking the bank.
May 2018 – The top stories in American healthcare continue to focus on our ever-increasing healthcare costs—costs that are nearly double those of other high-income countries while outcomes fall short on many population health measures[1]. And with no end to this upward spiral in sight, employers are grappling with how to continue providing their employees with high quality, affordable healthcare without breaking the bank.
Short Term Pain Relief
For the past few years, the go to lever for many employers has been to increase the cost burden of employees through benefit buy-downs and by moving them into high deductible plans. While temporarily holding back rising costs for employers, this strategy is losing steam as employees struggle to afford their increasing premiums and out-of-pocket costs while hampering their ability to access the quality healthcare their coverage is intended to provide for.
According to Milliman’s 2017 Medical Index, the average employee’s total cost share for PPO coverage for a family of 4 was roughly $11,500 per year (including premiums and out-of-pocket expenses).[2] Assuming that healthcare costs increase at 5.6% annually[3], in just 5 years that same family will be paying $15,000 per year for their healthcare. In the case of our self-insured employer trust, which serves the Dioceses of the Catholic Church, that would equal nearly 50% of the average priest’s annual salary.[4]
David Against So Many Goliaths
For a self-funded employer—even one of significant size such as ours with its 35,000 members—trying to control rising healthcare costs feels like an impossible task. What can one tiny David do when up against so many Goliaths—national health plans, big pharma, consolidating providers, federal and state regulators? And while these mega forces battle each other, employers are left with the unrelenting challenge of containing rising healthcare costs—not just for the sake of their employees but for the very mission each employer is trying to serve.
No Magic Bullets
So, what’s an employer to do? Unfortunately, there are no ‘magic bullets’ that can bend the slope of the medical trend line. Effectively managing healthcare costs requires a multi-pronged approach to driving change by developing a portfolio of initiatives designed to cumulatively reduce overall costs.
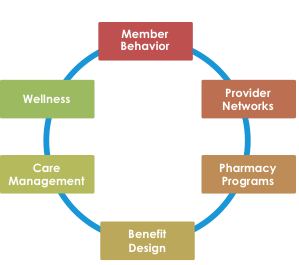
Given that the healthcare system is so complex, we found it helpful to try and simplify it. In the simplest terms, we focused on six basic levers that drive the cost of healthcare: member behavior, provider networks, pharmacy programs, benefit design, care management and wellness.
No Substitute for Hard Work
While most employers share similar cost characteristics, the process of developing an optimal portfolio of initiatives should begin with rigorous analysis. As the old saying goes, it pays to “follow the money” to identify the right potential solutions, keeping in mind having a bias towards low investment/high yield projects so the benefit streams can fund future initiatives. Another strategy to consider before initiating higher complexity (and therefore higher risk) projects is to take a page from Silicon Valley’s playbook—test and learn, fail fast and then scale up when you’ve discovered a solution that works.
Using this approach, our trust is on pace to reduce our costs by more than $10 million annually—or about 4% of our annual premiums. This result came by way of more than 20 discrete initiatives over the past 18 months; some were large, some were small, some we did on our own while others were done with partners, some were successful and a few failed. What they all had in common, though, was that they required intention and focused effort.
So, what worked for us? We began with good, old-fashioned negotiation, letting competition work for us. We started by developing a 36-month schedule for renegotiating our major vendor relationships, focusing our energy on the major spending categories. In a few markets, like reinsurance and pharmacy benefit management where markets are evolving quickly and competition is high, increasing the frequency of RFPs can yield substantial savings with relatively low effort. In our case, these negotiation efforts yielded nearly 50% of our overall savings with more expected to come in the near future.
The Curation Conundrum
When it came to reducing costs through more active management of member care, we found it challenging to identify and evaluate programs that would generate both the necessary financial benefit without adversely affecting quality of care – what we called our “curation conundrum.” Our existing partners all had extensive menus of cost-saving programs while dozens of start-ups were calling to offer their solutions. In order to solve this challenge, we only selected those partner-offered programs that could certify a demonstrable ROI and in cases where we took a risk on a new, innovative program, we limited our financial exposure to be able to “cut bait” if we failed to yield necessary results.
Reducing our pharmacy cost trend has been our single largest success to date. Working with our carved-out PBM, we have progressively added programs over time to contain costs while ensuring our members’ care was not adversely impacted, including: reference-based pricing, managed copayments, prior authorization, step therapy, specialty drug management, required mail order, centralized compounding, eliminating non-essential drugs, and stricter formularies.
While our portfolio approach has yielded strong results, the reality is that the rate that healthcare costs are increasing is still outpacing our efforts, leaving us with the certainty that our work will not be ending anytime soon.
About the Author:
Rob Geyer is health care industry executive with more than 25 years experience working in both for-profit and not-for-profit health plans. He currently serves as the Chief Executive for the Reta Trust, a self-insured employer trust providing health insurance to 35,000 employees of the Catholic Church. Previously, he was Senior Vice President of Customer Quality for Blue Shield of California, where he led the back-office and customer-facing operational functions of the plan serving more than 3 million members. A 4th generation native of California, Rob earned a BA in Economics from UC Davis and an MBA from Pepperdine University.
[1] Papanicolas I, Woskie LR, Jha AK. Health Care Spending in the United States and Other High-Income Countries. JAMA. 2018;319(10):1024–1039. doi:10.1001/jama.2018.1150
[2] Girod C, Hart S, Weltz S. 2017 Milliman Medical Index website. http://us.milliman. com/uploadedFiles/insight/Periodicals/mmi/2017-milliman-medical-index.pdf. Published May 2017.
[3] Centers for Medicare and Medicaid Services, Office of the Actuary. National health expenditure projections 2016–2025. https://www.cms.gov/Research-Statistics-Data- and-Systems/Statistics-Trends-and-Reports/NationalHealthExpendData/NationalHea lthAccountsProjected.html. Published February 15, 2017.
[4] Kramerek, M., National Diocesan Salary and Benefits Survey of 2017, The Center for Applied Research in the Apostolate at Georgetown, http://nineteensixty-four.blogspot.com/2017/07/earnings-in-catholic-church.html


Lorenzo Pizarro
Thank you. I appreciate you sharing the simplified framework of the six basic levers that drive healthcare costs – very helpful in simplifying something quite complex.